My LDC Benefits
Chronic kidney disease
Learn about kidney failure symptoms, tests, diagnosis and treatment options, including medication, dialysis and kidney transplant.
Overview
Chronic kidney disease, also called chronic kidney failure, involves a gradual loss of kidney function. Your kidneys filter wastes and excess fluids from your blood, which are then removed in your urine. Advanced chronic kidney disease can cause dangerous levels of fluid, electrolytes and wastes to build up in your body.
In the early stages of chronic kidney disease, you might have few signs or symptoms. You might not realize that you have kidney disease until the condition is advanced.
Treatment for chronic kidney disease focuses on slowing the progression of kidney damage, usually by controlling the cause. But, even controlling the cause might not keep kidney damage from progressing. Chronic kidney disease can progress to end-stage kidney failure, which is fatal without artificial filtering (dialysis) or a kidney transplant.
Signs and symptoms of chronic kidney disease develop over time if kidney damage progresses slowly. Loss of kidney function can cause a buildup of fluid or body waste or electrolyte problems. Depending on how severe it is, loss of kidney function can cause:
- Nausea
- Vomiting
- Loss of appetite
- Fatigue and weakness
- Sleep problems
- Urinating more or less
- Decreased mental sharpness
- Muscle cramps
- Swelling of feet and ankles
- Dry, itchy skin
- High blood pressure (hypertension) that's difficult to control
- Shortness of breath, if fluid builds up in the lungs
- Chest pain, if fluid builds up around the lining of the heart
Signs and symptoms of kidney disease are often nonspecific. This means they can also be caused by other illnesses. Because your kidneys are able to make up for lost function, you might not develop signs and symptoms until irreversible damage has occurred.
When to see a doctor
Make an appointment with your doctor if you have signs or symptoms of kidney disease. Early detection might help prevent kidney disease from progressing to kidney failure.
If you have a medical condition that increases your risk of kidney disease, your doctor may monitor your blood pressure and kidney function with urine and blood tests during office visits. Ask your doctor whether these tests are necessary for you.
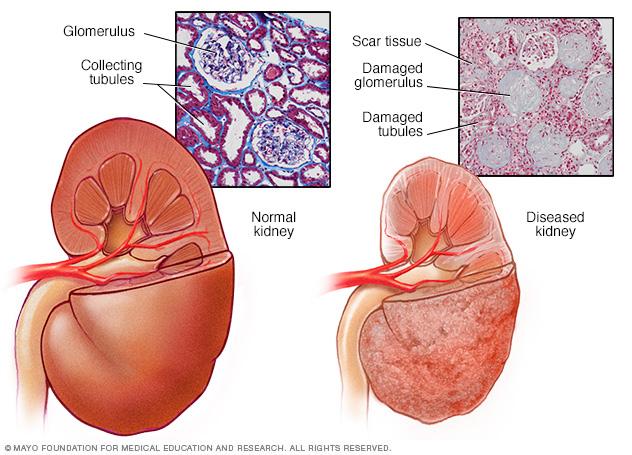
Healthy kidney vs. diseased kidney
A typical kidney has about 1 million filtering units. Each unit, called a glomerulus, connects to a tubule, which collects urine. Conditions such as high blood pressure and diabetes take a toll on kidney function by damaging these filtering units and collecting tubules and causing scarring.
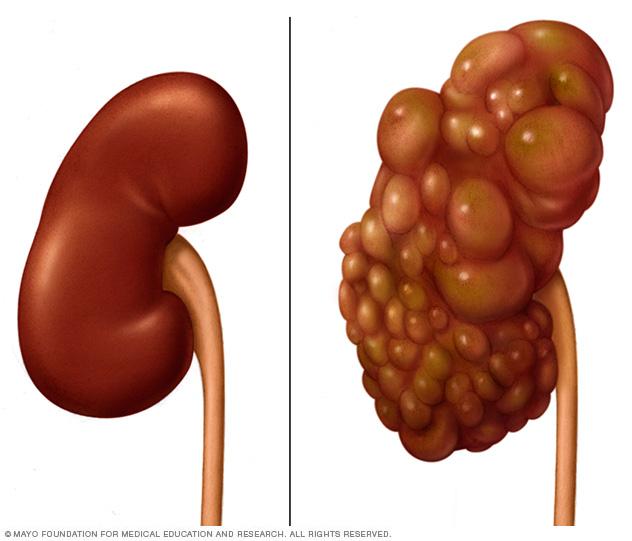
Polycystic kidney
A healthy kidney (left) eliminates waste from the blood and maintains the body's chemical balance. With polycystic kidney disease (right), fluid-filled sacs called cysts develop in the kidneys. The kidneys grow larger and gradually lose the ability to function as they should.
Chronic kidney disease occurs when a disease or condition impairs kidney function, causing kidney damage to worsen over several months or years.
Diseases and conditions that cause chronic kidney disease include:
- Type 1 or type 2 diabetes
- High blood pressure
- Glomerulonephritis (gloe-mer-u-low-nuh-FRY-tis), an inflammation of the kidney's filtering units (glomeruli)
- Interstitial nephritis (in-tur-STISH-ul nuh-FRY-tis), an inflammation of the kidney's tubules and surrounding structures
- Polycystic kidney disease or other inherited kidney diseases
- Prolonged obstruction of the urinary tract, from conditions such as enlarged prostate, kidney stones and some cancers
- Vesicoureteral (ves-ih-koe-yoo-REE-tur-ul) reflux, a condition that causes urine to back up into your kidneys
- Recurrent kidney infection, also called pyelonephritis (pie-uh-low-nuh-FRY-tis)
Factors that can increase your risk of chronic kidney disease include:
- Diabetes
- High blood pressure
- Heart (cardiovascular) disease
- Smoking
- Obesity
- Being Black, Native American or Asian American
- Family history of kidney disease
- Abnormal kidney structure
- Older age
- Frequent use of medications that can damage the kidneys
Chronic kidney disease can affect almost every part of your body. Potential complications include:
- Fluid retention, which could lead to swelling in your arms and legs, high blood pressure, or fluid in your lungs (pulmonary edema)
- A sudden rise in potassium levels in your blood (hyperkalemia), which could impair your heart's function and can be life-threatening
- Anemia
- Heart disease
- Weak bones and an increased risk of bone fractures
- Decreased sex drive, erectile dysfunction or reduced fertility
- Damage to your central nervous system, which can cause difficulty concentrating, personality changes or seizures
- Decreased immune response, which makes you more vulnerable to infection
- Pericarditis, an inflammation of the saclike membrane that envelops your heart (pericardium)
- Pregnancy complications that carry risks for the mother and the developing fetus
- Irreversible damage to your kidneys (end-stage kidney disease), eventually requiring either dialysis or a kidney transplant for survival
To reduce your risk of developing kidney disease:
- Follow instructions on over-the-counter medications. When using nonprescription pain relievers, such as aspirin, ibuprofen (Advil, Motrin IB, others) and acetaminophen (Tylenol, others), follow the instructions on the package. Taking too many pain relievers for a long time could lead to kidney damage.
- Maintain a healthy weight. If you're at a healthy weight, maintain it by being physically active most days of the week. If you need to lose weight, talk with your doctor about strategies for healthy weight loss.
- Don't smoke. Cigarette smoking can damage your kidneys and make existing kidney damage worse. If you're a smoker, talk to your doctor about strategies for quitting. Support groups, counseling and medications can all help you to stop.
- Manage your medical conditions with your doctor's help. If you have diseases or conditions that increase your risk of kidney disease, work with your doctor to control them. Ask your doctor about tests to look for signs of kidney damage.
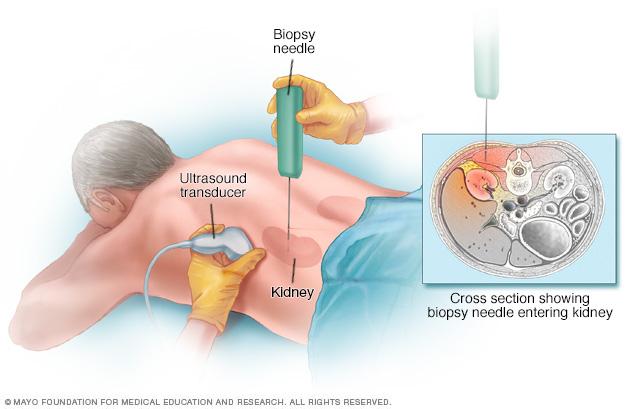

Kidney biopsy
During a kidney biopsy, your doctor uses a needle to remove a small sample of kidney tissue for lab testing. The biopsy needle is inserted through your skin and is often directed using the guidance of an imaging device, such as ultrasound.
As a first step toward diagnosis of kidney disease, your doctor discusses your personal and family history with you. Among other things, your doctor might ask questions about whether you've been diagnosed with high blood pressure, if you've taken a medication that might affect kidney function, if you've noticed changes in your urinary habits and whether you have family members who have kidney disease.
Next, your doctor performs a physical exam, checking for signs of problems with your heart or blood vessels, and conducts a neurological exam.
For kidney disease diagnosis, you might also need certain tests and procedures to determine how severe your kidney disease is (stage). Tests might include:
- Blood tests. Kidney function tests look for the level of waste products, such as creatinine and urea, in your blood.
- Urine tests. Analyzing a sample of your urine can reveal abnormalities that point to chronic kidney failure and help identify the cause of chronic kidney disease.
- Imaging tests. Your doctor might use ultrasound to assess your kidneys' structure and size. Other imaging tests might be used in some cases.
- Removing a sample of kidney tissue for testing. Your doctor might recommend a kidney biopsy, which involves removing a sample of kidney tissue. Kidney biopsy is often done with local anesthesia using a long, thin needle that's inserted through your skin and into your kidney. The biopsy sample is sent to a lab for testing to help determine what's causing your kidney problem.


Kidney transplant
During kidney transplant surgery, the donor kidney is placed in your lower abdomen. Blood vessels of the new kidney are attached to blood vessels in the lower part of your abdomen, just above one of your legs. The new kidney's urine tube (ureter) is connected to your bladder. Unless they are causing complications, your own kidneys are left in place.
Depending on the cause, some types of kidney disease can be treated. Often, though, chronic kidney disease has no cure.
Treatment usually consists of measures to help control signs and symptoms, reduce complications, and slow progression of the disease. If your kidneys become severely damaged, you might need treatment for end-stage kidney disease.
Treating the cause
Your doctor will work to slow or control the cause of your kidney disease. Treatment options vary depending on the cause. But kidney damage can continue to worsen even when an underlying condition, such as diabetes mellitus or high blood pressure, has been controlled.
Treating complications
Kidney disease complications can be controlled to make you more comfortable. Treatments might include:
-
High blood pressure medications. People with kidney disease can have worsening high blood pressure. Your doctor might recommend medications to lower your blood pressure — commonly angiotensin-converting enzyme (ACE) inhibitors or angiotensin II receptor blockers — and to preserve kidney function.
High blood pressure medications can initially decrease kidney function and change electrolyte levels, so you might need frequent blood tests to monitor your condition. Your doctor may also recommend a water pill (diuretic) and a low-salt diet.
- Medications to relieve swelling. People with chronic kidney disease often retain fluids. This can lead to swelling in the legs as well as high blood pressure. Medications called diuretics can help maintain the balance of fluids in your body.
- Medications to treat anemia. Supplements of the hormone erythropoietin (uh-rith-roe-POI-uh-tin), sometimes with added iron, help produce more red blood cells. This might relieve fatigue and weakness associated with anemia.
- Medications to lower cholesterol levels. Your doctor might recommend medications called statins to lower your cholesterol. People with chronic kidney disease often have high levels of bad cholesterol, which can increase the risk of heart disease.
- Medications to protect your bones. Calcium and vitamin D supplements can help prevent weak bones and lower your risk of fracture. You might also take medication known as a phosphate binder to lower the amount of phosphate in your blood and protect your blood vessels from damage by calcium deposits (calcification).
- A lower protein diet to minimize waste products in your blood. As your body processes protein from foods, it creates waste products that your kidneys must filter from your blood. To reduce the amount of work your kidneys must do, your doctor might recommend eating less protein. A registered dietitian can suggest ways to lower your protein intake while still eating a healthy diet.
Your doctor might recommend regular follow-up testing to see whether your kidney disease remains stable or progresses.
Treatment for end-stage kidney disease
If your kidneys can't keep up with waste and fluid clearance on their own and you develop complete or near-complete kidney failure, you have end-stage kidney disease. At that point, you need dialysis or a kidney transplant.
-
Dialysis. Dialysis artificially removes waste products and extra fluid from your blood when your kidneys can no longer do this. In hemodialysis, a machine filters waste and excess fluids from your blood.
In peritoneal dialysis, a thin tube inserted into your abdomen fills your abdominal cavity with a dialysis solution that absorbs waste and excess fluids. After a time, the dialysis solution drains from your body, carrying the waste with it.
-
Kidney transplant. A kidney transplant involves surgically placing a healthy kidney from a donor into your body. Transplanted kidneys can come from deceased or living donors.
After a transplant, you'll need to take medications for the rest of your life to keep your body from rejecting the new organ. You don't need to be on dialysis to have a kidney transplant.
For some who choose not to have dialysis or a kidney transplant, a third option is to treat your kidney failure with conservative measures. Conservative measures likely will include symptom management, advance care planning and care to keep you comfortable (palliative care).
As part of your treatment for chronic kidney disease, your doctor might recommend a special diet to help support your kidneys and limit the work they must do. Ask your doctor for a referral to a registered dietitian who can analyze your diet and suggest ways to make your diet easier on your kidneys.
Depending on your situation, kidney function and overall health, dietary recommendations might include the following:
- Avoid products with added salt. Lower the amount of sodium you eat each day by avoiding products with added salt, including many convenience foods, such as frozen dinners, canned soups and fast foods. Other foods with added salt include salty snack foods, canned vegetables, and processed meats and cheeses.
- Choose lower potassium foods. High-potassium foods include bananas, oranges, potatoes, spinach and tomatoes. Examples of low-potassium foods include apples, cabbage, carrots, green beans, grapes and strawberries. Be aware that many salt substitutes contain potassium, so you generally should avoid them if you have kidney failure.
- Limit the amount of protein you eat. Your registered dietitian will estimate how many grams of protein you need each day and make recommendations based on that amount. High-protein foods include lean meats, eggs, milk, cheese and beans. Low-protein foods include vegetables, fruits, breads and cereals.
Receiving a diagnosis of chronic kidney disease can be worrisome. To help you cope with your feelings, consider:
- Connecting with other people who have kidney disease. They can understand what you're feeling and offer unique support. Ask your doctor about support groups in your area. Or contact organizations such as the American Association of Kidney Patients, the National Kidney Foundation or the American Kidney Fund for groups in your area.
- Maintaining your normal routine, when possible. Try to keep doing the activities you enjoy and continue working, if your condition allows. This can help you cope with feelings of sadness or loss that you might have.
- Being active most days of the week. With your doctor's advice, aim for at least 30 minutes of physical activity most days of the week. This can help you cope with fatigue and stress.
- Talking with someone you trust. You might have a friend or family member who is a good listener. Or you may find it helpful to talk with a faith leader or someone else you trust. Ask your doctor for a referral to a social worker or counselor.
You'll likely start by seeing your primary care doctor. If lab tests reveal that you have kidney damage, you might be referred to a doctor who specializes in kidney problems (nephrologist).
What you can do
To get ready for your appointment, ask if there's anything you need to do ahead of time, such as limit your diet. Then make a list of:
- Your symptoms, including any that seem unrelated to your kidneys or urinary function, and when they began
- All your medications, vitamins or other supplements you take, including doses
- Other medical conditions you have and relatives with kidney disease
- Questions to ask about your condition
Take a family member or friend along, if possible, to help you remember the information you receive. Or use a recorder during your visit.
For chronic kidney disease, some basic questions to ask include:
- What's the level of damage to my kidneys?
- Is my kidney function worsening?
- Do I need more tests?
- What's causing my condition?
- Can the damage to my kidneys be reversed?
- What are my treatment options?
- What are the potential side effects of each treatment?
- I have these other health conditions. How can I best manage them together?
- Do I need to eat a special diet?
- Can you refer me to a dietitian who can help me plan my meals?
- Are there brochures or other printed material I can have? What websites do you recommend?
- How often do I need to have my kidney function tested?
Don't hesitate to ask other questions as they occur to you.
What to expect from your doctor
Your doctor is likely to ask you questions, such as:
- How long have you had symptoms?
- Have you been diagnosed or treated for high blood pressure?
- Have you noticed changes in your urinary habits?
© 1998-2023 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved.


